How COVID-19 is shaping lives in Liberia



Dr. Mary Yang, from Toronto, ON, completed her psychiatry residency at University of Toronto in June 2019. After residency, she began a fellowship with Partners In Health, whose work she had followed since high school, and went to Liberia as PIH’s 2019-2020 Dr. Mario Pagenel Global Mental Health Delivery Fellow. She is now back in Toronto and shares her reflections with PIH Canada.
In October 2019, I travelled to Liberia and began getting to know the dedicated, selfless members of PIH’s mental health team in Harper, Liberia. To get to Harper, you travel first to Monrovia, Liberia’s capital, then from there if you have the time (and patience, and physical stamina), you take a 4×4 vehicle over two days on bumpy roads to Harper. The alternative is a one-hour bush plane flight that operates three times a week.
Harper is in Maryland County in the very southeast corner of the country, with close links to Ivory Coast in terms of food, supplies, and people regularly crossing the border. It has the faded glamour of a resort town that saw its heyday in the 1970s, and waves perfect for a beginning surfer. In Maryland County, PIH supports the two largest health facilities, JJ Dossen Hospital in Harper and Pleebo Health Centre. Pleebo is a bigger town often bustling with traders and commerce from the Ivory Coast, including food imports.

My work in Liberia consisted of accompanying my Liberian mental health colleagues with the goal of improving the mental health care system. There are only two psychiatrists in Liberia, both working in Monrovia. Most of the workforce are mental health clinicians trained in the WHO’s Mental Health Gap Action Programme (mhGAP). Our clinics see about 600 patients per month. For me, this meant sitting with clinicians as they patiently and tirelessly saw patients, day after day, in cramped conditions. Most of our patients had epilepsy. In Liberia, as in many places in the world, epilepsy is considered a mental health problem. My Liberian colleagues were surprised that European and North American clinicians don’t consider epilepsy a mental health condition, which led to interesting discussions on what exactly constitutes mental health versus physical health.
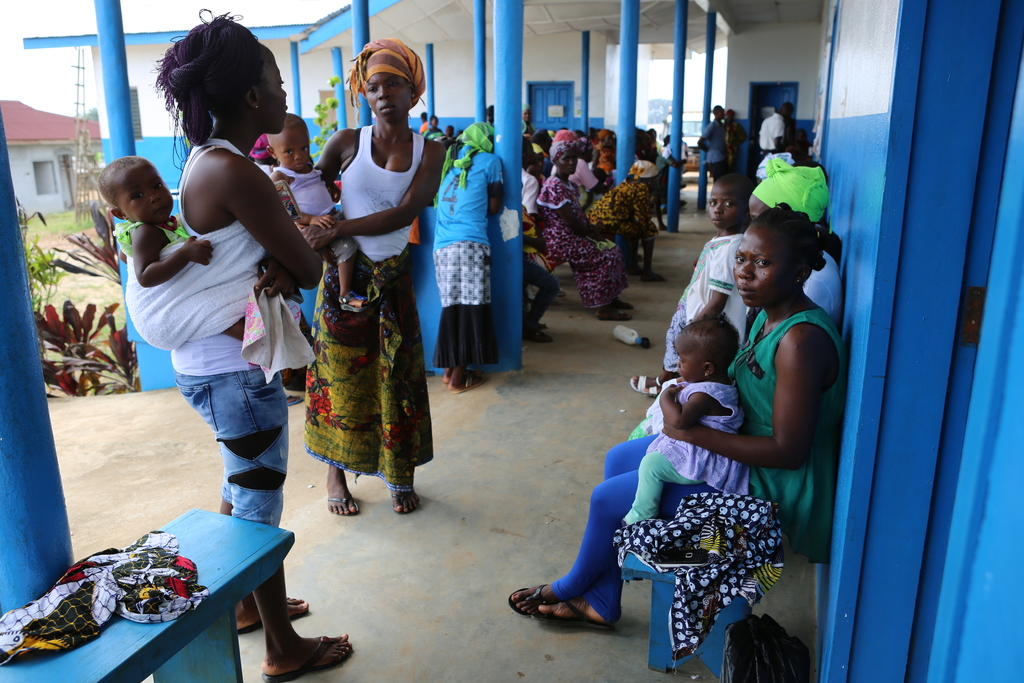
Most patients at JJ Dossen or Pleebo depend on day-to-day labour for their income. They’re often uncertain where their next meal is coming from. Patients with mental health problems are at even higher risk, because they often cannot perform the same day-labour activities and are more dependent on others for food and money. Most people share their homes with several family members. It was moving to see how important medical care was for families; patients would regularly travel on foot from distances as far as the Ivory Coast, sometimes with children on their backs, to seek care for their loved ones.
I was on vacation in Europe in late February when coronavirus hit. After consulting with senior leadership, we decided it would make sense for me to “wait out coronavirus” in Canada; this was at the very early days of the pandemic when most European countries and Canada had fairly low case-counts. Liberia had strict entry requirements due to COVID-19 concerns early on. Several days after arriving back in Toronto, we realized that the virus was going to be a problem everywhere. Liberia saw its first case in the middle of March, and PIH turned its attention to COVID-19 response.
In all the ways that my life has changed due to COVID-19 in Toronto, it frightens me more to think about how it will affect the lives of colleagues, friends, and patients in Liberia. Going to the grocery store can be stressful, but I am more grateful than ever that we have intact, robust supply chains for food. In Liberia, the border with Ivory Coast was closed on March 24. Since then, people in Harper have seen increases in the price of food and reductions in availability. The rainy season has started, so soon the roads from Harper to Monrovia will be flooded and the county will be effectively cut off from the rest of Liberia for months. Already people are facing terrible decisions about whether to protect their health or their livelihood. And just as in Canada, Liberia has seen fewer people coming to hospital for urgent health needs, and precious resources and personnel have been assigned to COVID-19 from their usual clinical duties. The true impact – lives lost from untreated mental health conditions, chronic medical conditions, lack of antenatal care – may not be known for years.

My Liberian colleagues still have fresh memories of the Ebola virus disease, which ended in 2015. Terms such as social distancing and IPC (infection prevention and control) were familiar to them. But COVID-19 is not Ebola. The usual donor countries are dealing with their own catastrophes. Yet we have much to learn from the experience of countries like Liberia: the importance of community health workers, mass contact tracing, and responding to stigma. We should also not forget that our Liberian partners need resources, funds, and solidarity more than ever. The playing field is not fair, and never has been. The world’s biggest powers are using every means possible to procure PPE for themselves, for example – and this inequity can have devastating consequences for my colleagues working every day to serve those in need.
Your support for PIH Canada will help us ensure that the voices, perspectives and lives of our partners are not forgotten in the midst of this global crisis.



