Improving Cervical Cancer Treatment in Haiti

With more clinical options, women gain access to free, lifesaving care
Posted on June 1, 2022

Shortly after Haitian President Jovenel Moïse was assassinated in July 2021, Belennda Joseph noticed an odd discharge leaking from her vagina. At first, she thought it was stress: the country had descended into turmoil, violence escalated, and citizens were on edge. But two weeks later, when she noticed some blood, Joseph made an appointment to see an OB-GYN in Port-de-Paix, where she lived. The doctor said she was anemic, prescribed medication, and sent her home without performing an exam.
But the bleeding didn’t stop, said Joseph, speaking in Haitian Creole through a translator. Over the next several months, through a maze of new doctors, delayed test results, and rising concerns, Joseph finally got a diagnosis: cervical cancer. It was stage 2, she learned–too advanced to remove surgically.
The news hit her hard, she said, “it broke my heart.” Even though cervical cancer is the leading cause of cancer-related deaths among women in Haiti, Joseph, 31, formerly a nurse at the University of Notre Dame Hospital in Port-de-Paix, said she’d never known another woman who had it. That’s not unusual in a country where treatment has been scarce and diagnosis can be spotty. Women with cervical cancer—many young, in their 30s or 40s— are often left to fend for themselves, doctors say, sent home with pain medication only, left to suffer, and eventually die.
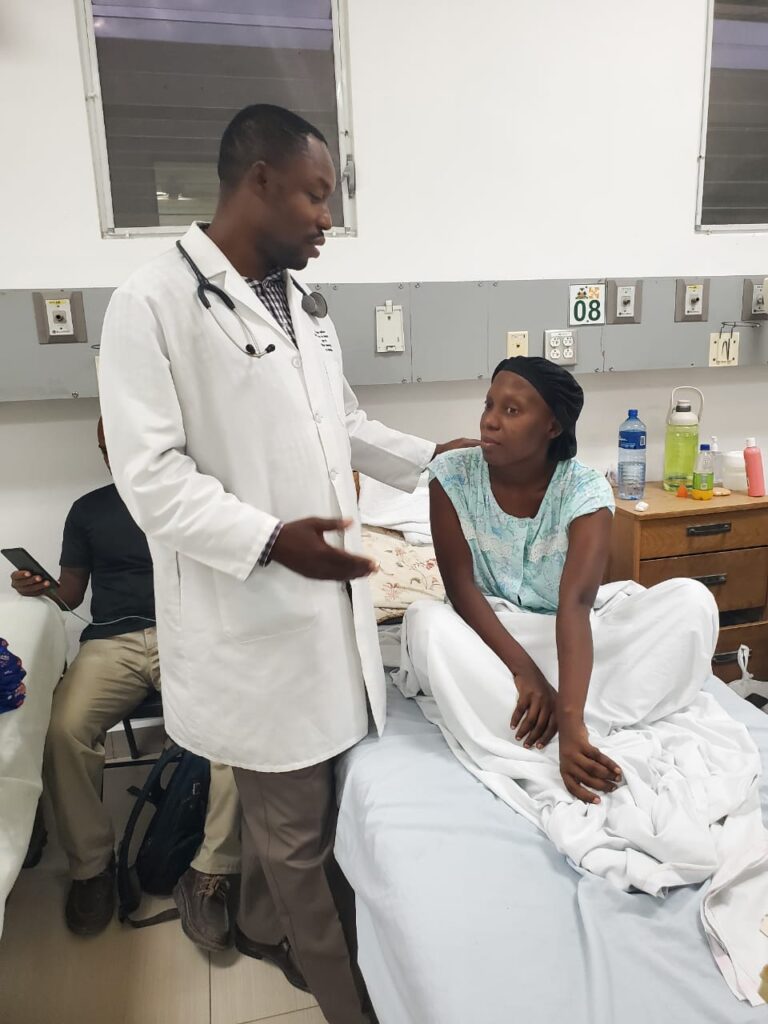
In wealthy countries, cervical cancer is highly preventable through routine screening, like pap smears, and with HPV vaccines. In Haiti, however, where Zanmi Lasante–PIH’s sister organization–has worked for decades, such screening is not part of primary care; nor are the many mainstays of gynecological cancer treatment, such as radiation or a full menu of chemotherapy drugs. And, with no fellowship-level gynecological oncology training for clinicians, there are few specialists in the country to treat such cancers.
A $10,000 Treatment—in Another Country
The doctor who delivered Joseph’s diagnosis did suggest one option: travel to the Dominican Republic, where more extensive treatment would be available. “Get a passport as soon as possible,” he’d said. She considered this until she spoke to clinicians in Santo Domingo, who informed her that the cost of radiation treatment would be about $10,000. For her family of five siblings and a single mother whose farm was decimated due to drought, that price tag, in a country where the gross income per capita is about $1,250, was completely out of reach.
All the while, Joseph continued bleeding.
What Joseph didn’t know at the time was that for just over a year, an interdisciplinary team of clinicians from Zanmi Lasante’s Hôpital Universitaire de Mirebalais (HUM), Dana Farber Cancer Institute in Boston, AdventHealth in Florida, University Hospital in Kinshasa, and Massachusetts General Hospital (MGH) and Harvard Medical School had been meeting weekly over Zoom to discuss a range of gynecologic cancers afflicting patients in Haiti. The global team was launched to broaden and support local clinicians’ capacity to care for patients with gynecological cancers, including ovarian, endometrial, vulvar, and others, with particular attention to cervical cancer. In the weekly case conferences and monthly deep dives with experts, clinicians discuss new treatment options and emerging research and bring together specialists to work through difficult cases. For instance, a recent discussion centered on a complex case of gestational trophoblastic disease with a world-class expert, a Harvard pathologist, and local Haitian doctors, led by Dr. Christophe Millien, an OB-GYN and medical director of HUM. The new collaboration also initiated “telepathology” consults in which pathologist volunteers in Boston review samples from Haitian patients.
So far, the team has discussed about 50 complex cancer cases. At HUM, more than 20 cervical cancer patients have been treated under the new global consult system led by Millien, and OB-GYNS Dr. Jean Clause Ulysse, and Dr. Jean Joel Saint Hubert.
Improving Care, Now and Into the Future
The evolution of cancer care at HUM has a familiar PIH arc: Rather than accepting the constraints of the setting—no radiation, a severely limited blood supply which impedes major surgeries, no gynecological cancer specialists—the team instead is thinking creatively, scouring the medical literature for evidence-based alternatives to improve care. At the same time, clinicians continually strategize on how to build a system that supports even more robust care in the future.
For example, Dr. Tom Randall, a gynecologic oncologist at MGH, and associate professor of obstetrics, gynecology, and reproductive biology at Harvard Medical School, cites a research study out of India which led to a paradigm shift in care.
The study, by researchers at the Tata Memorial Centre in Mumbai and published in the Journal of Clinical Oncology in 2018, involved 635 patients with cervical cancer. Patients were assigned into two groups: one received neoadjuvant chemotherapy (that is, giving chemo first) followed by surgery; the other group received the standard of care, chemotherapy plus radiation. While the radiation patients showed slightly better survival rates, the gap was not huge: Researchers reported the 5-year disease-free survival in the chemotherapy plus surgery group was 69.3% compared with 76.7% in the chemo plus radiation group.
For Haiti, that’s good news, said Randall: the Tata study shows that it’s possible, in resource-poor settings where radiation is unavailable, to provide cervical cancer patients a viable treatment option. “The study demonstrated that neoadjuvant chemotherapy followed by radical surgery is a feasible, safe, and effective treatment for locally advanced cervical cancer when radiotherapy is not available,” he said.
A Radical Shift
For Millien, at HUM, the ability to provide this improved level of care is a radical shift.
“I can testify to the difference,” he said. “At first, when I got a cervical cancer patient, I could not do anything for her—no care. Now it’s different, now there is something we can do.”
HUM is one of the first centers in the world to incorporate this approach to cervical cancer treatment in a very low-resource setting.
And so, when Joseph showed up at HUM early one morning last November to wait at the front of the line outside the facility, she met with Millien, who said he could try to treat her cancer. “How much would it cost?” she asked. He replied: “It’s free.”
The road would not be easy: Multiple rounds of harsh chemo, surgery to remove her uterus, and reliance on others to care for her through recovery, loss of her job. All of this made Joseph nervous, unsure about whether to proceed with her treatment. But Millien told her it was a question of life and death. “God is arranging one thing after another for me,” Joseph said. But then she re-evaluated her options and agreed to the surgery. She met with Dr. Joarly Lormil, the chief of oncology, psychologists, and social workers, who reassured her that she’d be taken care of at HUM. After three rounds of chemotherapy, the mass still had not shrunk enough to operate, so Joseph needed an additional three rounds.
On March 11, Joseph underwent surgery. Despite some post-operative complications, Millien said, the procedure went well. Joseph, in the end, said she is glad to now move forward.
She said that since she was unable to travel outside Haiti for treatment, without this surgery “the cancer would have eaten me, and I would have died.”
To ensure better, and more comprehensive care in Haiti for others like Joseph, facing gynecological cancer, the international consortium is still pushing the boundaries of what’s possible. Ultimately, the goal is to make radiotherapy available more widely in Haiti, but this is likely to take many years.
For now, clinicians are working to develop a deeper bench of specialists who can manage these complex cancer cases. Patients in wealthy countries take for granted the availability of gynecological oncologists, but in Haiti, no such training program existed—until now. In late April, it was announced that the Mirebalais University Hospital Gynecologic Oncology Fellowship in Haiti, the first of its kind in the country, had been approved by the International Gynecologic Cancer Society. Now that the fellowship is official, the international consortium will work to finalize its global curriculum and mentorship fellowship based at HUM. “Our plan is to ultimately train one to two residents each year,” said Rebecca Henderson, an MD/PhD candidate at the University of Florida, who has been working with the team since its inception in early 2021.
Randall of MGH said the program will provide Haiti’s first comprehensive two-year education and training program in gynecologic oncology by pairing Haitian trainees with expert mentors who track the trainees’ progress. The plan is for mentors to eventually travel to HUM biannually to provide trainees with hands-on surgical training, and fellows will likewise complete one to three months of clinical observation at the mentor’s institution.
After several weeks of recovering from surgery, and various complications due to her advanced cancer, Joseph was discharged from HUM in early April.
“Cancer prognoses are always uncertain and good outcomes are never guaranteed,” Millien said. “In Haiti, where many of the mainstays of cancer care are missing and diagnoses are often made late, this is especially the case. Belennda can at least know she has a care team who is going above and beyond to provide everything they can in this resource-limited setting.”
Originally published on pih.org



