Need to Know: MUAC and Malnutrition

Spend a day at any Partners In Health site and there’s a good chance you’ll hear a phrase you’re unfamiliar with. Perhaps it’s a clunky acronym or polysyllabic drug name. But don’t worry: Keeping up with the ever-evolving world of global health is hard, even for insiders. In Need to Know, we cut through the complexity and deliver the most pertinent and interesting information on a single subject. Today, we fill you in on mid-upper arm circumference.
What is it?
Mid-upper arm circumference, often shortened to MUAC, is a measurement that allows health workers to quickly determine if a patient is acutely malnourished. PIH, as well as many other organizations, measures the circumference of a patient’s arm at the midpoint between his or her shoulder and elbow.
Why is it important?
The burden of malnutrition is staggering. According to a series of articles in The Lancet, more than 3 million child deaths every year are associated with malnutrition. Put another way, nearly half of all children who die each year do so because they don’t have access to enough of the right food. Our health workers in Haiti, Malawi, Lesotho, and Rwanda, among other locations, encounter malnourished patients every day. MUAC provides a fast and effective screening method.
How do you make the measurement?
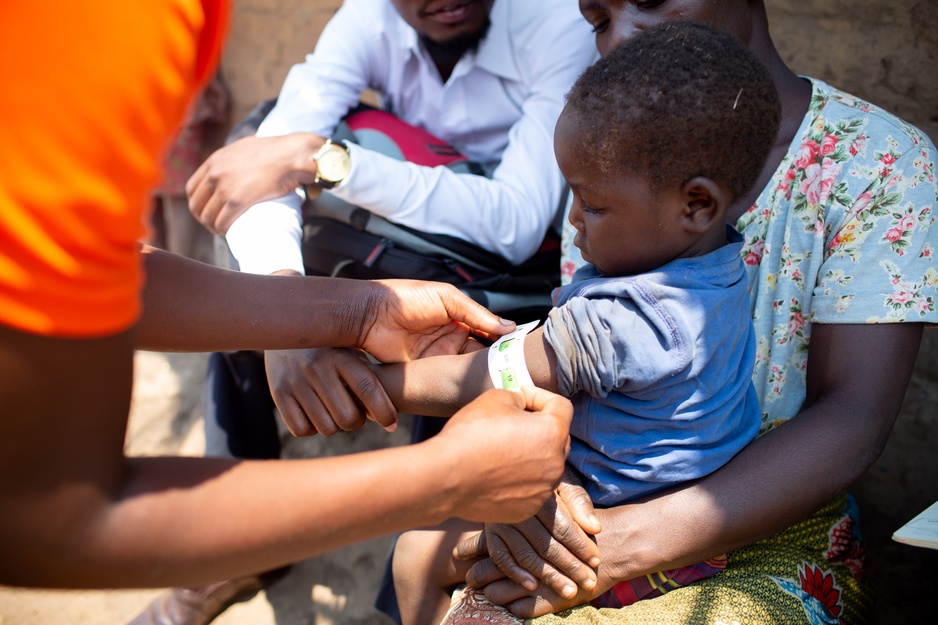
There are specific paper MUAC bands that are colour-coded. If the girth of the patient’s arm falls within the green part of the band, it indicates that the patient is not malnourished. A measurement that falls within the yellow part of the band indicates that the patient may be at risk of malnutrition. Lastly, the red portion of the band indicates that the patient is severely malnourished and at risk of death. Some bands include a fourth colour, orange, which indicates the patient is moderately malnourished.
What happens after the measurement is taken?
Well, that depends on the measurement. Generally, if a child is malnourished, we provide treatment with ready-to-use therapeutic food, commonly known as RUTF. These foods are high in fat and protein and fortified with the vitamins and minerals necessary to treat severe acute malnutrition. A few weeks of treatment with RUTF can bring about significant improvements. PIH will often take steps to improve the long-term food security of patients’ families. This might include enrolling people in job training, delivering food assistance, or providing materials for farming.
Malnutrition is a complex problem. Is a paper arm band all you’re using in the fight against it?
Absolutely not. MUAC is an immensely helpful tool but it’s not foolproof. For instance, a simple arm measurement doesn’t tell us whether a patient has kwashiorkor, or protein malnutrition. Furthermore, the accuracy of MUAC diminishes as the child ages. That’s why we’re constantly devising and implementing new ways to alleviate the root causes of malnutrition and catch malnourished children earlier.
In Malawi, for instance, we conduct regular community malnutrition screenings to identify young patients who haven’t been able to travel to clinics, which are sometimes hours away by foot from their family home. Meanwhile, in Haiti, we opened a facility in 2013 that has dramatically scaled up the production of Nourimanba, a ready-to-use therapeutic food made from locally grown peanuts. PIH produced 165,000 pounds of the nutritional supplement last year alone. MUAC is merely one part of a comprehensive strategy that helps us make proper diagnoses and act accordingly.

Article originally posted on pih.org



