Research: Doctor Investigates HIV/AIDS Therapy Patterns at Hospital in Haiti

Younger patients, those struggling to meet basic needs more likely to have trouble with medication regimen
Posted on Aug 8, 2022

Ludentz Dorcelus clearly recalls the “complete chaos” that overwhelmed his hometown of Port-au-Prince after a 7.0 magnitude earthquake devastated Haiti in 2010, killing some 300,000 people. Dorcelus, 18 at the time, was one semester short of graduating high school when the quake, which leveled the capital city, hit.
In order to finish school, Dorcelus and his parents agreed that he would move to the U.S., to the home of an aunt and uncle, in Nanuet, NY—a small town about 30 miles north of Manhattan. There, he graduated, then returned home and passed the local exams to complete high school in Haiti and apply to college, settling on a career in medicine. Now, Dorcelus is in the final year of his residency: he plans to stay in Haiti and practice family medicine.
Education was a focus of his family, Dorcelus said, so it’s not surprising that when it came to structuring a research project as part of his medical school “social service” year, his hypothesis was that education was closely correlated with adherence to medication protocols. “A lot of that was based on my own experience,” he said.
However, the results of his research, which looked specifically at adherence to antiretroviral therapy (ART) at one hospital in Haiti and was published in the journal AIDS Research & Therapy last November, undermined that theory. For Dorcelus, the study’s lead author, that finding came as a “big surprise.”
Research Findings
The study included 411 patients at St. Therese Hospital in Hinche, a public facility in central Haiti, which is also supported by Zanmi Lasante, Partners In Health’s sister organization. Zanmi Lasante, founded in the early 1980s, now comprises a network of 15 clinics and hospitals in some of the country’s most impoverished regions and serves more than 1.3 million people.
Researchers, relying on self-reported patient data, found that age and the ability to meet basic needs were the only two factors that significantly correlated with adherence. “The odds of having poor adherence was significantly higher in patients under 40 years compared to those 40 years of age and older,” the study concluded. Additionally, it found: “Patients who could not meet their basic needs were more likely to have poor adherence.”
Earlier research has also found that younger patients can have more trouble following medical protocols in similar settings, Dorcelus said. That body of work suggested that older patients were more accustomed to the routine of medical regimens: “The survival instinct was also mentioned in these studies: the elderly patient, in decline, recognized that their life expectancy would be prolonged through good adherence.” At the younger end of the spectrum, “adolescents and young adults were at increased risk of treatment failure due to multiple social, psychological and adherence barriers,” the recent study had found.
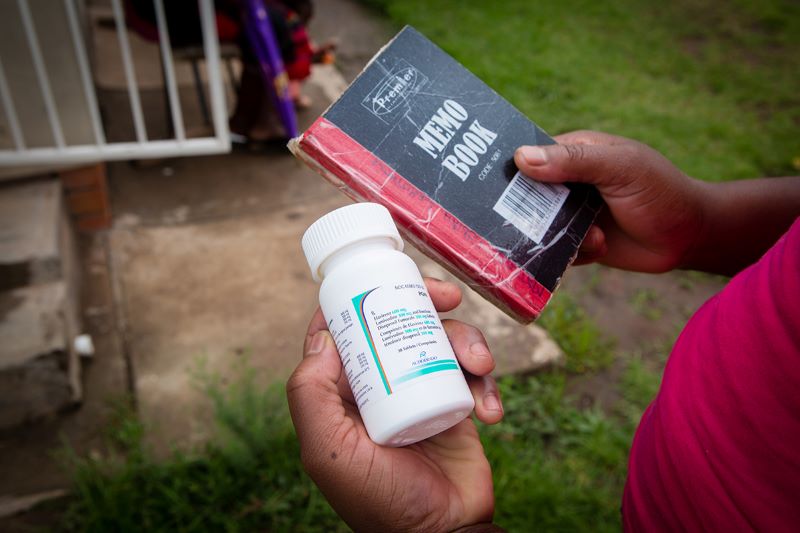
Better Outcome and Survival
Adherence matters when it comes to all medications, but in particular, it’s associated with better outcomes and survival among people living with HIV, the study noted.
To be sure, most patients in the study —a full 82%— reported their adherence to ART was “excellent.”
Among those who reported poor adherence, the reasons varied, but many of them stemmed from general poverty: “Only 9% said they could always meet their basic needs compared with 27.9% who could never meet their needs. Not being able to meet their basic needs was associated with almost three times greater odds of poor adherence.”
The study noted that ART is free in Haiti. “Were treatment not free, it would likely pose an even greater barrier to treatment adherence,” the study said. “If they [patients] do not have enough resources for food, they are likely to be more focused on solving this immediate need, instead of achieving viral load suppression. It is also a common belief amongst Haitians that medication should not be taken on an empty stomach. Living in poverty, not having access to water/food may prevent them from taking their medication.”
More Studies Needed
And while other studies have shown a link between education and adherence, this one did not. The literacy rate in Haiti for those 15 and older is 61%, the study noted, and the Central Plateau region has the nation’s highest illiteracy rate. “Surprisingly,” the authors said, “we found no statistically significant difference between adherence among those that had been schooled compared with those who had received no schooling.” However, they theorized that given the high illiteracy rate and limited ability to meet basic needs, “it is likely that access to education could potentially improve adherence to ART in this area.”
Overall, Dorcelus said, more studies— at more hospitals— are needed to figure out all of the complex elements that drive adherence. “We need a nationwide study or a larger study to figure out the other barriers,” he said.
The Importance of Social Support
Dorcelus’ driving curiosity in the research struck Mary Clisbee, provost for academic affairs and research at the University of Global Health Equity in Haiti. “What I find most amazing is that he recognized the problem, searched the literature, and developed the study on his own, and during his service year!” Clisbee said. “That is unheard of! His level of motivation and autonomy is remarkable.”
Dr. Ornella Sainterant, director of medical education at HUM adds: “This study proves once again Dr. Paul Farmer’s teaching on social medicine [and] medical humanism: Our treatment won’t work without social support.”
For now, Dorcelus said he is working on another project looking at the factors linked to poor glycemic control in diabetic patients, while also finishing up his studies. Though his future career path is not clear at this point, one thing is certain.
“Even though the situation is bad, people are fleeing the country, and we are living in constant fear,” he said, “I grew up in Haiti. I want to stay here and serve my population.”
Originally published on pih.org



