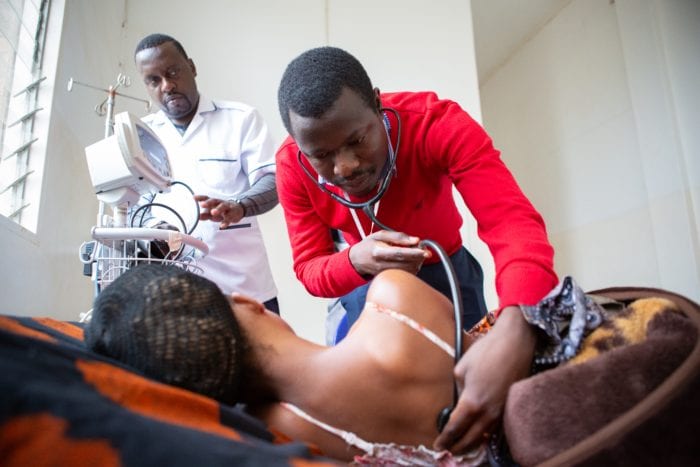
A Cancer Crisis, A Good Solution


at the Butaro Ambulatory Cancer Care Center in Burera District, Rwanda. (Photo by Calvin Kennell-Heiling for Partners In Health)
Since 2012, a Partners In Health-supported public hospital in northern Rwanda has treated thousands of patients for breast cancer, lymphomas, and more. But even Butaro Hospital has struggled to treat late-stage cancers and other conditions needing radiation therapy. Like many developing countries, Rwanda lacks a $4 million radiation therapy machine.
So clinicians at the hospital refer patients to Mulago Hospital in Kampala, Uganda, and accompany them on the 300-mile bus trip there. Or rather, they used to. In April, Mulago’s 20-year-old, second-hand radiation therapy machine broke. Experts soon declared it unfixable, and tens of thousands of cancer patients from Uganda, Burundi, South Sudan, and Rwanda were suddenly left without treatment.
Partly in response to this, the government of Rwanda pledged to open a radiation therapy service. Uganda has also said it will. But neither facility is likely to be ready within a year and a half, let alone immediately, which is of course what patients need.
Clinicians at Butaro were not content to wait. They went looking for options available now. Of the handful of radiation therapy machines within a 1,500-mile radius of Butaro, they settled on referring patients to one in Nairobi, Kenya. The private hospital is topnotch, and relatively close, just 500 miles away.
In the letter below, Dr. Alex Coutinho, the executive director of PIH’s program in Rwanda, describes visiting Nairobi and meeting the first radiation therapy patients, and he explains why spending $6,000 per patient is a terrific deal.
Dear colleagues,
This letter is from Nairobi, Kenya, where I am to finalize arrangements for radiation therapy service for our cancer patients for the next two years. Some of my management team members—Neil Gupta, Paul Park, Cyprian Shyirambere, and Antoinette Habinshuti—had done a great job identifying the right provider and negotiating the right discounted price for PIH. My time here has been used to evaluate the services provided and finalize the wording of the legal document that will guide our relationship with The Nairobi Hospital, as well as meet the Rwanda embassy in Nairobi to ensure that they are aware we have referred patients and that they can provide support if needed.
Most important, though, was to meet the very first five beneficiaries of the new radiation therapy service. The five exemplify the characteristics of the people we serve in Rwanda—mainly women, almost all from rural areas, and probably from the poorest of the poor categories. I could sense that The Nairobi Hospital had no experience dealing with an organization like PIH, one that prioritizes the poor and offers them sophisticated medical services usually far beyond the reach of even the middle class in Rwanda.
I found the five women huddled in a group outside, sitting on the grass and basking in the sun on a chilly morning. Three of the women are Catholic, another is Pentecostal, and the fifth is a Muslim, which highlights the diversity in Rwanda and the fact that all religions co-exist very well there. (I had to find out the religions to arrange a pastoral service for them if they needed it). I had a long conversation with them through an interpreter and their main concerns were about the unfamiliar food, about the exact nature of the treatment they were receiving, and of course about whether they would be cured. Yet overall they were upbeat and excited. They had flown in an airplane to come to Nairobi and much preferred it to the arduous journey they had had on a bus to and from Uganda when their first radiation therapy quest went awry. I asked them if there was anything else they wished for. And I was so surprised that they requested a tour of Nairobi city. They wanted to have “stories to tell their relatives when they get home.” In keeping with the ethos of the Make-a-Wish Foundation, arranging a tour of Nairobi city and Nairobi safari park is now my task. The five live in a hostel just across the road from the hospital and are in clean, comfortable accommodations with plenty of food and drinks. However they are not used to city traffic so crossing the busy road requires an escort.
Our oncology program in Rwanda has helped nearly 5,000 people since it started in 2012 but one can only understand its impact when one speaks to an individual beneficiary, hearing their thoughts, their anxieties, their aspirations, and their hope for a “second life.”
The program in Nairobi is not cheap. The radiation therapy program alone costs $6,000. If one adds the chemotherapy, pathology, biopsy, etc. that we perform in Butaro, then the unit cost of caring for one patient who receives radiation therapy is closer to $10,000. I can recall when this was the unit cost for Anti-Retroviral Therapy in the U.S. and very very few Africans could access it. And I recall the frustration I felt then, as my patients, my friends, and even my relatives perished of AIDS. Today the unit cost of ART in Rwanda is about $450 per year, and if the normal life expectancy of that HIV+ individual is increased by 30 years, then the lifetime ART cost will be $13,500. Therefore if we can achieve an oncology cure for these five women with $10,000 and gain 20 additional years of life for them then the costs would have some equivalence.
And yet this is not primarily about cost. This is about not giving up when faced with the “conventional wisdom”—that ART will not work in Africa because we don’t have watches or that oncology is not scalable because of complexity and cost. Well, in The Nairobi Hospital, I had a tour and saw a state of the art radiation therapy unit with two linear accelerators, a brachytherapy unit, an MRI and CAT scan dedicated for staging and planning therapy, and a team of Kenyans managing this complex. This is what Rwanda aspires to have in the coming years and what we want in Butaro or Kigali, to be able to provide universal health coverage, including oncology patients.
So PIH referring patients to Nairobi at great cost is a call to action, a demonstration that no obstacle is permanent, and it’s a rally cry for the global health community to respond to the cancer crisis that is looming in the developing world. But in the end, it is about women and men and children like these five, about their lives, and the lives of their families and children and loved ones.
My last letter highlighted the continuing challenges PIH will face, in partnership with the Rwandan Ministry of Health, in trying to meet the need and demand at all of our sites, and the need for oncology services at all out sites. We know that for now we cannot meet all the need, but we can attempt to respond compassionately, and we can attempt to help those that somehow, against all odds, find their way to our facilities. I am truly uplifted to be part of PIH as we take on this oncology challenge. I am also thankful to the generous supporters around the world. As the proverb goes, “People who say it cannot be done should not interrupt those who are doing it.”
Have a great week,
Alex