Cholera’s Toll Continues in Haiti with Children Most Affected
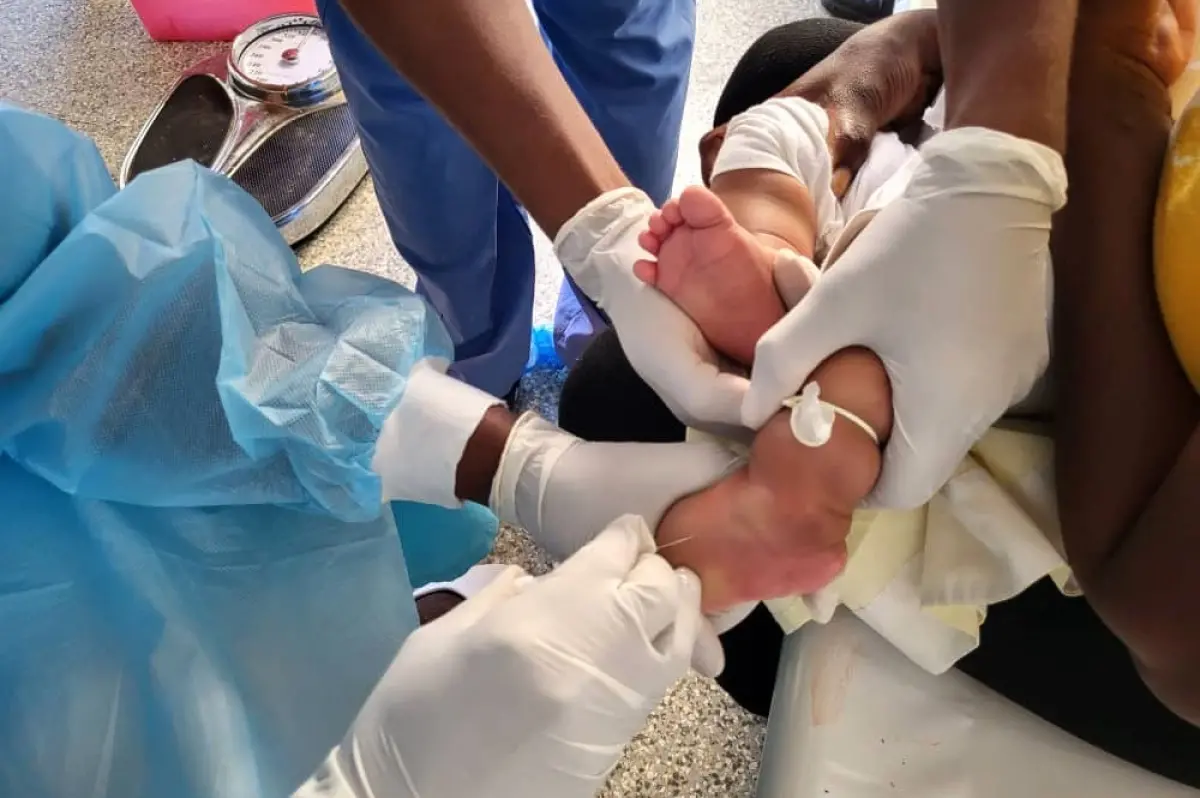
Treatment centers open amidst malnutrition, ongoing challenges
Posted on December 21, 2022
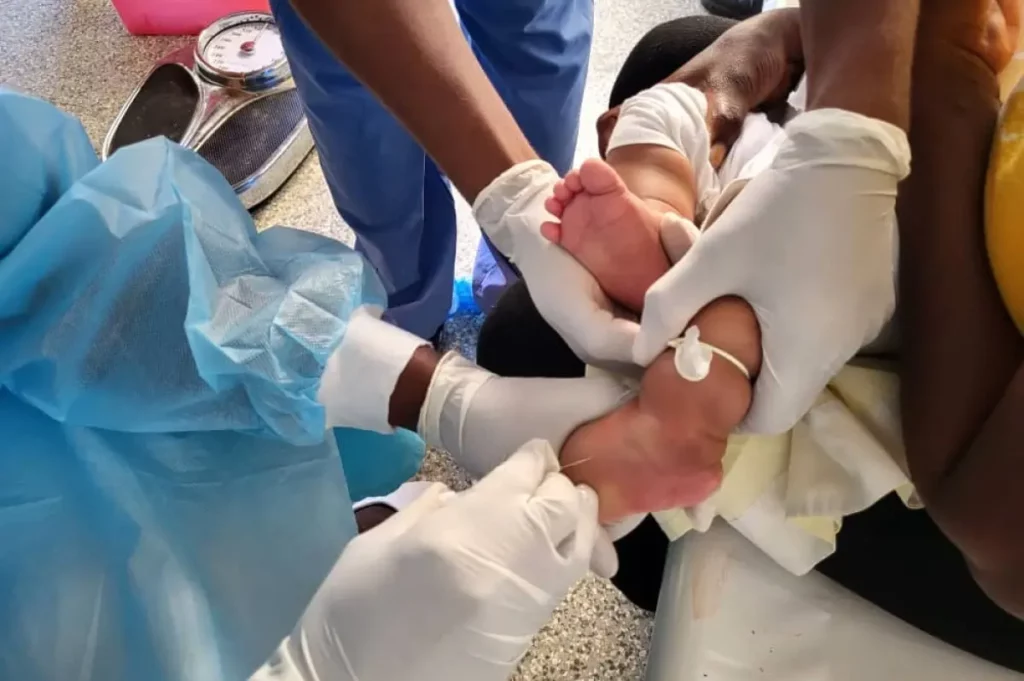
As the latest cholera outbreak in Haiti continues, its impact is clear: children under 5 have been most affected.
As of December 6, the Haitian Ministry of Public Health and Population (MSPP) reported 13,586 suspected cases of cholera, 11,670 hospitalizations, and 285 fatalities. The unofficial toll is likely even higher.
Early on, clinicians noted that children were hardest hit by the disease, which causes diarrhea and vomiting and, when severe, can lead to fatal dehydration within 24 hours.
Widespread Malnutrition
“We were asking ourselves this question: ‘Why are children the main victims of cholera?’” said Dr. Jean Joel Manasse, an internal medicine physician and head of the cholera treatment unit at Hôpital Universitaire de Mirebalais (HUM), which is supported by PIH’s sister organization in Haiti, Zanmi Lasante, and built in partnership with the MSPP. Now, even as the percentage of adults with cholera rises, children remain the majority of cases, about 65%, Manasse said.
One reason is widespread malnutrition. “A significant proportion of children with cholera also have associated malnutrition,” which, Manasse explained, tends to leave young immune systems more vulnerable to disease. “Those [cholera patients] with longer hospital stays face a risk of complications such as acute lung edema, infection, limb edema,” and other problems associated with severe malnutrition, he added.
Malnutrition is on the rise in Haiti. According to The New York Times, “the United Nations reported [in October] that for the first time ever, hunger, which has long haunted Haiti, had reached “catastrophic” levels in the Cité Soleil neighborhood” of Port-au-Prince, among the most impoverished areas of the capital city. That designation is the most extreme level of hunger, which has left thousands facing famine-like conditions, the article stated, noting that some residents have resorted to drinking rainwater and making meals out of boiled leaves.
At HUM, physicians are initiating malnutrition treatment right at the cholera treatment centers, Manasse said, and then ensuring that children are referred to pediatricians and enrolled in the hospital’s nutrition program.
Dire Working Conditions
Staff continue to treat patients despite a country plagued by gang-related violence, kidnappings, rampant inflation, and ongoing shortages of fuel and other necessities.
At Zanmi Lasante, Executive Director Marc Julmisse said the teams at HUM and five other ZL-supported clinics continue to work around the clock to provide cholera care, despite daily challenges.
“On September 12, our country came to a standstill,” said Julmisse, speaking about conditions in Haiti as part of a PIH global health webinar in November. “We had been dealing for years with kidnappings, gang violence, roadblocks, but this is unprecedented. We haven’t seen it before.”
Julmisse talked about the risks staff face simply getting to and from work, and acquiring much-needed fuel which, at its worst, was being sold for $20 a gallon due to countrywide shortages. “We had to make some tough decisions just to keep the doors open,” she said.
But the doors have remained open, she added, as cholera cases keep rising.
The first official case was on October 2. Within two weeks that number jumped to 66 cases. Now, case reports from the Ministry of Public Health and Population tick upwards daily.
At HUM, the 60 beds for cholera patients quickly filled up; there were 200 patients being treated as of December 7 with a total of about 1,000 cholera patients have been cared for and treated at HUM, a state-of-the-art teaching hospital built following Haiti’s devastating 2010 earthquake.
Julmisse said the ZL team is actively working on opening new cholera treatment sites around the region and collaborating with medical and health care organizations throughout Haiti to strategize on how best to treat patients and save lives.
This cooperation, she said, is critical: “It’s like, ‘What do you have, what do we have, can we share?’” she said. “We have formed a community of proactive groups to better understand what’s going on, each advocating for each other.”
For instance, she said, it became clear that the community of Lascahobas was facing an increase in cases, but many patients living in remote, rural locations could not make the trek to clinics for care. This information was relayed to community health workers, and plans are now underway to get teams to that area to help residents who are sick.
Recently, Airlink, an organization that works with partners, including Zanmi Lasante, to deliver crucial supplies during humanitarian crises, has established an “airbridge” to get water, sanitation, and hygiene supplies to Haiti to mitigate the outbreak.
“We are in a dire situation,” Julmisse said. “But we have an amazing team.”
Dr. Christophe Millien, medical director at HUM, said several new general practitioners and a pediatrician have been hired to help manage the cases. But critical needs for additional cholera treatment centers remain, notably: tents, beds, oral rehydration salts, IV and hygiene supplies, and more.
Importantly, PIH and ZL, alongside government partners, are anticipating the oral cholera vaccine to arrive in Haiti on December 12, with a coordinated vaccination campaign launching two days later, officials said.

Cholera’s History in Haiti
Cholera had not been detected in Haiti until after the 2010 earthquake, when it was inadvertently introduced by United Nations security forces, sickening 820,000 people and causing almost 9,800 deaths. After multiple, successful mass vaccination campaigns led by PIH and others, and a decision by the World Health Organization to create a cholera vaccine stockpile, cholera was declared eliminated from Haiti in February 2022.
However, according to a recent analysis in The New England Journal of Medicine, the reemergence of the disease was caused, at least in part, “by a descendant of the [cholera] strain that caused the 2010 epidemic.”
The authors of the NEJM piece, including those affiliated with PIH, suggest several explanations: that the original strain persisted undiagnosed in the population and recurred “in the context of waning population immunity coupled with a crisis in lack of clean water and sanitation;” that the strain persisted in environmental reservoirs; or that the current strain could have been reintroduced in Haiti from a nearby country.
In any case, the authors conclude: “These findings, along with the resurgence of cholera in several parts of the world despite available tools to fight it, suggest that cholera control and prevention efforts must be redoubled.”
Originally published on pih.org



