One Year Into Pandemic, Honouring the Strain, and Triumph, of Nurses
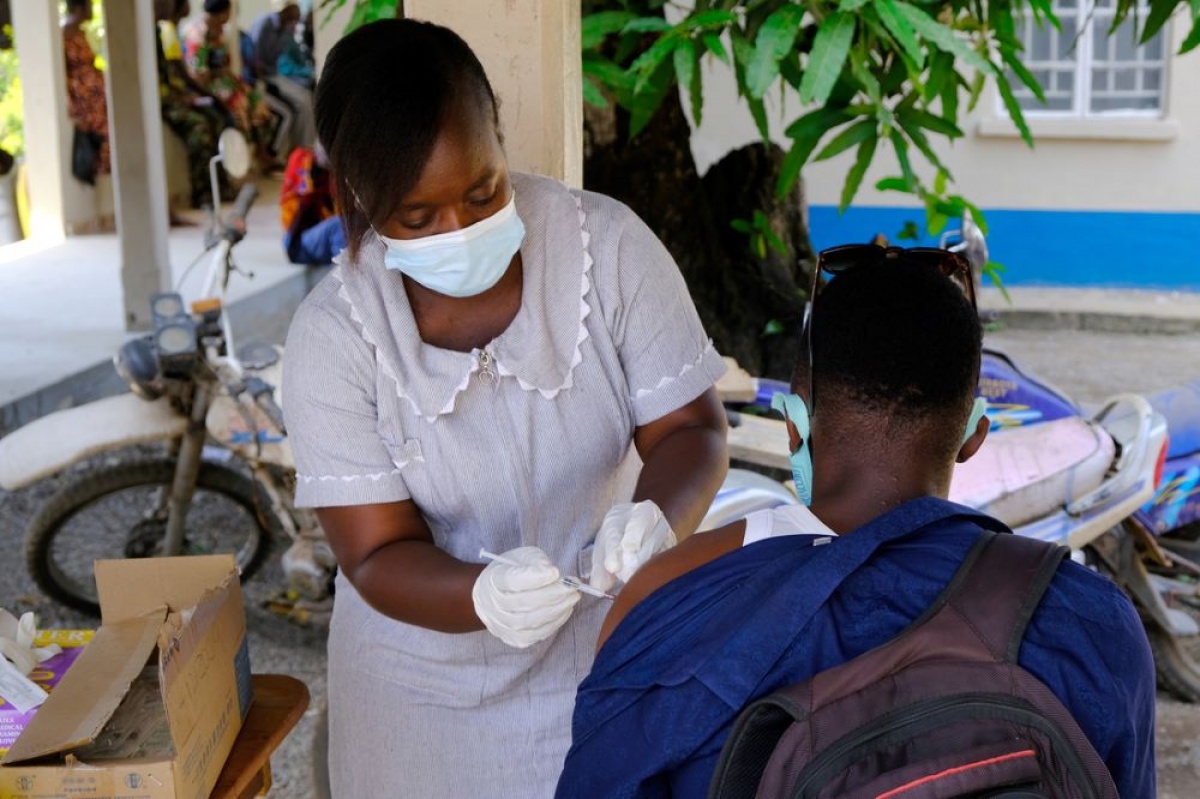
Nurses as essential workers confronting COVID-19, and life’s everyday emergencies
Posted on May 6, 2021
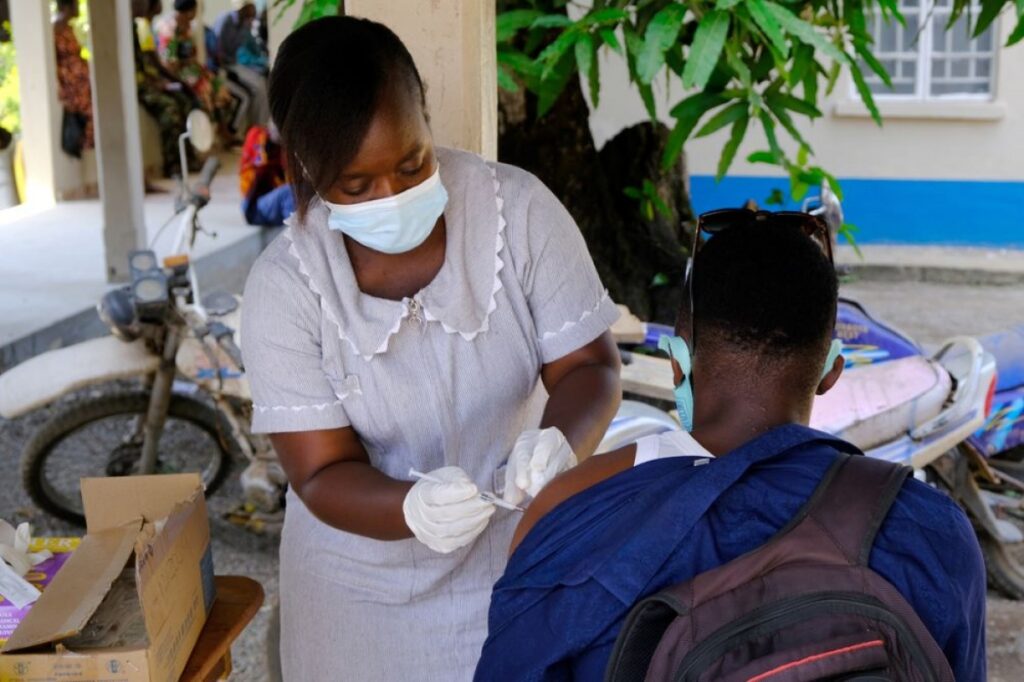
In honour of National Nurses Week, the following essay was co-authored by Partners In Health CEO Dr. Sheila Davis; Cory McMahon, deputy chief nursing officer; and Judy Khanyola, chair of nursing and midwifery at the University of Global Health Equity in Rwanda.
As individuals, as communities, and as a society, this past year has forced us to reflect on many things with new perspective—not least of which the importance of nursing globally. COVID-19 brought into sharp focus the critical role nurses have played in confronting this pandemic.
Think of the array of images shown on a daily basis. Nurses held their patients’ hands as they took their last breath, isolated from friends and family. Nurses helped the mother in labour deliver her baby safely. Nurses gave chemotherapy to grateful patients, because cancer does not pause for COVID-19. Nurses visited patients’ homes to ensure they received essential care, linking them to social services and referring them to hospitals when needed. Nurses managed with makeshift personal protective equipment when there was not enough at hospitals and clinics.
Always, nurses were—and are—the first to jump in, giving themselves wholeheartedly during a very challenging and uncertain time.
COVID-19 has wreaked havoc on our health care systems across the world, demonstrating our interconnectedness, exacerbating health inequities, and giving visibility to the essential role of nurses. The nursing workforce is the world’s largest occupation in the health sector—at 27.9 million strong and 59% of health personnel. Nurses are essential to delivering on the promise of universal health care, as they provide an overwhelming 90% of health services globally.
At Partners In Health, 50% of the clinical workforce are nurses and midwives. Nearly 90% of our more than 1,200 nursing and midwifery staff are female. They are leaders and decision-makers, patient advocates and care providers, cherished colleagues and good friends. They are there when disaster strikes, and they are there for life’s everyday emergencies.
Early on in the pandemic, nurses were deeply involved in assessing and putting into place infection prevention and control measures and readying facilities and systems to care for an exponential increase in patients. For more than a year, they have been caring for the critically ill, working in uncertain conditions against a relatively unknown virus, all while lacking essential PPE and putting their own and their families’ lives at risk to care for others. Meanwhile, nurses have remained trusted members of their communities, often serving as the bridges between patients and health care systems.

As we enter this next phase of the pandemic, nurses are additionally being asked to take on massive global vaccination efforts. Rwanda exemplifies the lift required of nurses in that effort. The country plans to vaccinate a third of the population in 2021 and reach 60% by the end of next year. Within three weeks of the first vaccine’s arrival in Rwanda, more than 348,000 people had received their first dose. The majority of those vaccinations were administered by nurses.
By 2030, it is estimated that there will be a global gap of 5.7 million nurses. That number was arrived at pre-pandemic—before nurses suffered what should have been an unbearable level of personal and professional stress and burnout—and is likely now much higher.
Despite its challenges, nursing has always been a profession that is united; we rise together and support each other for the betterment of our patients. For us, one of the highlights of this past year has been watching PIH nurses and other health care professionals from Liberia, Rwanda, Haiti, Lesotho, Sierra Leone, Malawi, Mexico, Peru, and the United States learn from each other and engage in a meaningful exchange of ideas, successes, and challenges. This pandemic has helped us, once again, intimately understand the interconnectedness of our work. And that’s why we must continue to fight for the rapid and equitable global rollout of COVID-19 vaccines, because no one is safe, until everyone is safe.
We know our most powerful pandemic preparedness efforts are to educate, employ, and invest in nurses as essential care providers within health systems. This means ensuring nurses receive a quality education, are fairly compensated, have career pathways, and are able to practice to the full extent of their licensure. Nurses must also serve as critical members of decision-making teams, ensuring patients’ concerns remain at the center of care.
Nurses have been essential to quality care from the early days of this pandemic, stayed steady—though strained—through surge after surge, and remained standing in solidarity with each other and their patients. Let’s remember, when these long days are over and we reach a new normal, that nurses are more than first responders in times of emergency; they are natural leaders who, regardless of conditions, get the job done.
As of late March, all PIH-supported countries in Africa—Lesotho, Liberia, Malawi, Rwanda, and Sierra Leone—have received their first batch of vaccines from COVAX. Most countries have kicked off their vaccination campaigns, and they’re all prioritizing health care workers, including community health workers, then individuals older than 65 and those with chronic conditions. As of March 26, about 10,000 people in Sierra Leone had been vaccinated with a single dose; 13,000 in Lesotho; 348,000 in Rwanda; and 71,000 in Malawi.
Article originally published on pih.org.



