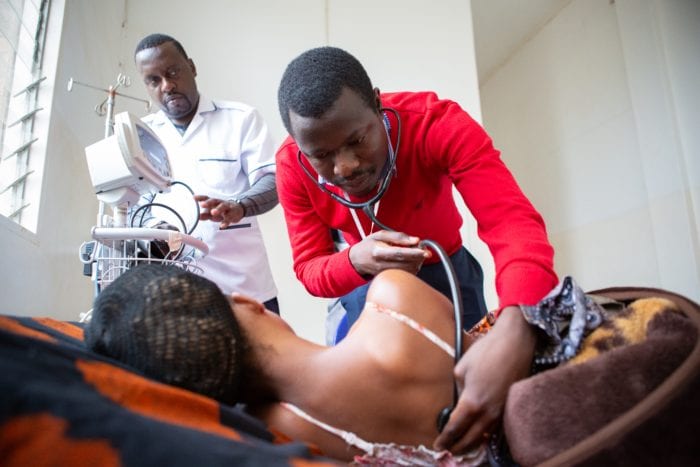
Pediatric Development Clinic Helps High-Risk Babies in Rwanda


Pictured: Maria Kaitesi/Partners In Health Janet Kayitesi, caretaker for baby Diane Uwamahoro, plays with the child as part of the Pediatric Development Clinic run by the Rwandan Ministry of Health and PIH/IMB. Photo: Maria Kaitesi/Partners In Health
Infant survival has steadily improved in Rwanda over the past decades. But mere survival isn’t enough for Rwanda’s Ministry of Health and Partners In Health’s sister organization, Inshuti Mu Buzima. They aim to ensure that high-risk babies have every opportunity to thrive.
To work toward this goal, the Ministry of Health and PIH/IMB have created the Pediatric Development Clinic with support from UNICEF and specialists from Boston Children’s Hospital. The interdisciplinary program is intended to improve health outcomes for babies at risk of death or developmental delays. It’s the first program of its kind in Rwanda.
The clinic started in April 2014 in Rwinkwavu District Hospital and has since expanded to Kabarondo and Ndego health centers. Staff have enrolled 123 infants who were born prematurely or with low birth weight, perinatal asphyxia, or other complications such as suspected genetic syndromes and developmental delays. The babies’ families receive services that include group education, peer support, and social worker assessments.
“Some mothers are always on the verge of giving up, thinking their children are about to die,” said Olivier Bigirumwami, nurse in charge of the clinic at Rwinkwavu District Hospital. “But through the counseling services we offer, we manage to educate them about the conditions of their children, how they can play their part while we also play our medical part. There has been massive improvement in the lives of the children under 5.”
The Ministry of Health and PIH/IMB conducted an early assessment of the program, collecting feedback from the mothers and caregivers who participated with their children.
“When I came here, I talked with the social worker and clinician, and they made me feel comfortable,” one mother said. “Before, I thought that the child would not be alive. I thought the child would die at any time. Now I feel comfortable, and I love my child.”
The Pediatric Development Clinic is one of many PIH/IMB efforts focused on child health. PIH/IMB identified the need for the clinic while improving overall care for preterm and low-birth-weight babies at health facilities, PIH/IMB Director of Pediatrics Dr. Hema Magge said. Complications from prematurity are the No. 1 cause of death for children 5 and younger globally, she said.
“Currently, there’s no systematic way to know what happens with [high-risk infants] after hospital discharge,” she said. “Yet, we know that they are at increased biologic risk of medical, nutritional, and developmental issues, and that early detection and early intervention can optimize their quality of life and prevent long-term complications.”
The clinic allows health care providers to follow these babies after they go home, through regular clinic appointments and community-based support.
The program features a weekly nurse-led clinic at health facilities, social supports such as food and transportation money for vulnerable families, and training for staff members in caring for high-risk infants through simple interventions. High-risk families are identified by social workers and receive home visits and community-based support as well. The program also is linked with electronic medical records systems to improve care and tracking of patients.
But beyond the clinic’s medical benefits, Magge sees the program as a step toward improving the lives of rural Rwandans.
“It’s really about breaking cycles of poverty,” she said. “You’re using this target population of medically vulnerable infants to shift the entire early childhood development agenda forward. … We want a generation of healthy, active children, going to school, getting educations, and getting out of poverty. That’s what this is all about.”
PIH/IMB hopes to add Pediatric Development Clinic programming at two more clinics in 2015 and is exploring the possibility of working with the Ministry of Health to replicate it on a national scale. Dr. Fulgence Nkikabahizi, Rwinkwavu District Hospital’s medical director, said one challenge has been making sure the model is affordable.
“Plans are under way to conduct a costing study and see how sustainable this program is,” Nkikabahizi said. “We want to assess the real cost, own it as Rwandans, and scale it up at national level in the near future.”
Scaling up the clinic would expand access to a unique program.
“We don’t know of any other models for long-term follow-up and intervention support for high-risk infants in resource-limited settings in rural, non-referral settings without specialists,” Magge said.
The Pediatric Development Clinic includes training for nurses, social workers, and doctors who might encounter high-risk babies. After infants are enrolled, they will continue to participate in the clinic for varying amounts of time, depending on their condition. Magge expects babies and families to receive clinic services until the children reach at least age 2 and up to age 5. Children who need specialized care after age 5 will be referred to other PIH/IMB-supported chronic care programs.
The clinic’s goal for most infants is to intervene during a key developmental stage and help them catch up to their peers.
When babies and their caregivers visit the clinic, Magge said, the caregivers learn how to interact and play with the children to promote development. One caregiver reported using those lessons at home:
Before, I thought my child couldn’t learn anything, but now after visiting PDC clinic, I try to teach my child things like, “This is a cup.” I repeat the word to the child over and over again, then after a few days I can say, “Look at the cup,” and the child sees it and shows that he understands. Now I sit with my child to teach him. This is a big difference. Before coming here I did not know I should do this. I knew the child has a very big disability and thought he could not learn. Now I see that he can still learn.
The early program assessment suggests caregivers and staff members are enthusiastic about the clinic. It also found that caregivers of high-risk babies face barriers, such as transportation challenges, lack of family support, and the stigma of being seen as unable to care for a child.
To address these concerns, PIH/IMB and the MOH plan to add weekend support groups and to increase the number of home visits, engaging fathers and other family members in the care of these children.