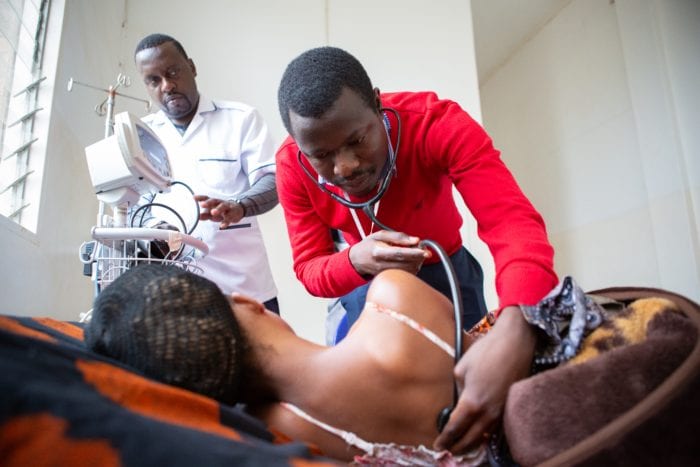
Shaping Family Medicine in Haiti
Dr. Kerling Israel is Director of Medical Education for Partners In Health / Zanmi Lasante, and is Program Director of PIH/ZL’s Family Medicine Residency program at Hospital Saint Nicolas in St. Marc. This summer, Dr. Israel visited Toronto to take part in the TIPS-FM course (Toronto International Program in Strengthening Family Medicine and Primary Care), hosted by Department of Family and Community Medicine at the University of Toronto. Partners In Health Canada spoke with Dr. Israel to learn how her work is helping to shape the future of medical education in Haiti.

Could you tell us a little bit about the TIPS-FM program at U of T that you are currently a part of?
I am a learner. We’re a small group here, and we try and better understand how University of Toronto runs its family medicine residency program. While Haiti has been inspired by the US model of residency programs, I wanted to gain a different perspective as well as build new relationships. This is a great opportunity to learn things that I can use to improve my program in Haiti.
What inspired you to get involved in medicine?
I don’t know if I was really interested in medicine from the beginning, but I knew that I was interested in people and helping them in some capacity. As I grew up, I began to realize that I could do a lot of service in the medical field and that it was also an opportunity for me to combine my interest in education and teaching.
As director of the family medicine residency program in St. Marc, what does a typical day look like?
Since January, my role has changed a bit, but when I was the full-time program director, my day would consist of getting together with the residents in the morning for our academic activity for about an hour, and then follow-up and review of programmatic activity. Because it is a fairly new program, you have to review the curriculum on an ongoing basis and manage the vision that is being set through constant communication with your staff. So my day would be part clinical, part teaching and part management.
What do you hope to accomplish with the family residency program?
We wanted to create a new model of medical education for Haiti. We structured the program so that we would be working closely with the national medical school. We’ve put a lot of emphasis on the importance of evaluation, so we’ve structured the program in a way that requires the evaluation of our residents, of the teachers, and of the program itself by the residents. After a year and a half, we also had an internal review done. These are perhaps common things to do in other programs, but for Haiti, it is new. It is a huge step when you can ask individuals to come and see what you’re doing and get feedback. We also have visiting professors from the national medical school as well as from Universities in the US mostly who give us ongoing feedback as to how we are doing. Now, two years on, as a result of its success, this program has become well known across Haiti – The Ministry of Health mandate Zanmi Lasante /PIH to take on medical education at University Hospital in Mirebalais using the Hospital Saint Nicolas Family Medicine Residency Program model. The success of the program has built the legitimacy required to move forward and build other residency programs in Mirebalais.
Would you say that building that foundation is one of the things you’re most proud of?
Yes, but I am also proud of the social justice attitude I see in my residents. While I know that they are clinically very good, I am proud of them because I can see that they are also interested in making changes. They have become very interested in working on quality improvement projects and research, two things that are very new in Haitian medical education. They understand the message that they are not just doctors, but that they can be agents of change while practicing medicine and working within their communities.
The quality of care that Zanmi Lasante provides is important not just for the individual patient, but for the hope that you can contribute to elevating standards across the country. Do you get a sense that this is happening?
We are trying to achieve this on multiple levels. The first thing is that we try to help the Ministry of Health and the national medical school whenever we can. For example, you will find us as advisories for Haiti’s national HIV working groups, or when they have to review training curriculum.
The second aspect is working directly with medical students. When they come to our hospital sites we can teach them about equity of care through social and community medicine and emphasize how important it is. At the last national conference on quality improvement, Hospital Saint Nicolas won two prizes. One was for a project done by one of my residents and the other one was awarded to the hospital staff. This is one way to show people that even though you don’t have a lot of resources, you can still make incremental changes to improve things. Over time, the senior residents no longer view problems and think “Oh, we cannot solve it.” Now they say, “Okay, let’s see where the problem is and try to fix it.” I think this is a very important cultural shift that has occurred. It has made people feel welcome and that together, they can do something great.
What do you see in the future for the residency program?
There are a few things that we envision for Mirebalais. First, we really have become big partners with the Ministry of Health and the national medical school in supporting medical education. Currently, we are helping to build a research department and develop a kind of continuing education curriculum for teachers. We would really like to continue this kind of work to help strengthen the national medical school. The other priority is to try and share our resources with other patients and residents who do not have direct support from PIH so everyone can benefit. For example, if an internal medicine specialist or emergency room doctor could come to Mirebalais for rotation, they could be trained on how to interpret images from a CT scan or how to use an ultrasound machine. This is specific and structured training that we would like to provide to them.
Another thing we continue to work towards in regards to our residents is incorporating the philosophy of the organization into their training and practice. In other words, having them enter into the program to become not just family doctors or go on to specialize, but to be imbued by a sense of responsibility to help the poor and make the community stronger. We hope that with this mindset, they will be willing to go into more rural areas and be willing to bring the resources with them as opposed to saying “I will not go there because there aren’t any resources.”
If we continue to receive financial support for this program to train family physicians after 10 years and even before that, we will start seeing the transformation of the primary care delivery and real change in the health system of this country to the benefit of the population.
Seventy percent of our specialists are in Port-au-Prince. We want to shift this. Being outside of Port-au-Prince opens you up to a great experience, but the second thing is to help the residents understand that this is something we can change, that thinking about those less fortunate and wanting to provide them with high quality care is critical to the success of providing equitable care to the people of Haiti.