Groundbreaking Kazakhstan TB Trial Continuing Amid COVID-19 Challenges
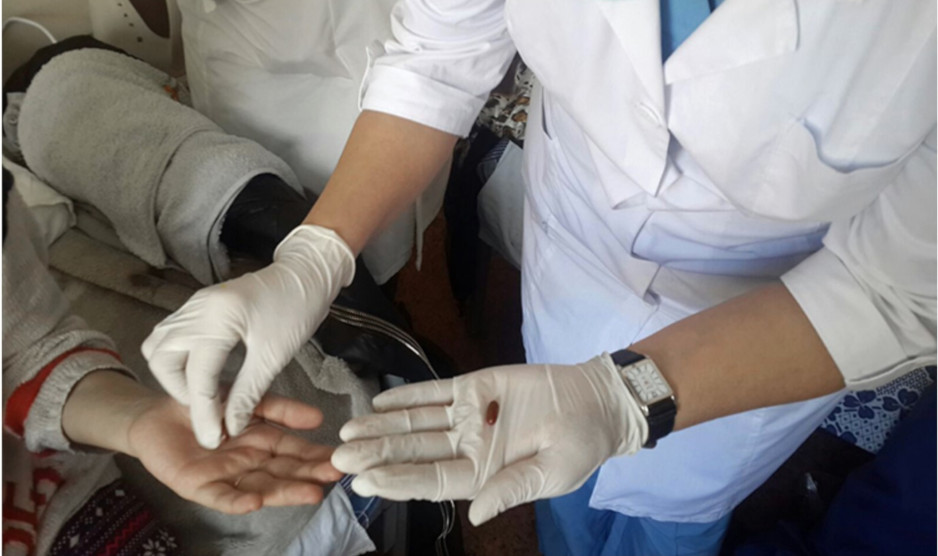

Despite Kazakhstan’s nationwide lockdown that began in March to contain COVID-19, Partners In Health clinicians have continued to examine and provide treatment—in person and online—for tuberculosis patients enrolled in a groundbreaking clinical trial.
Clinicians have had to communicate regularly with police to cross checkpoints and have used their own vehicles as testing sites, checking patients’ vision, hearing, and hearts for treatment-related side effects from the seat of a car.
Kazakhstan is one of seven countries participating in the clinical trial for the endTB partnership, a multi-year, international effort to fight the world’s deadliest infectious disease. It’s the biggest TB trial in the world, led by PIH and conducted in partnership with Médecins sans Frontières, Interactive Research & Development, and financial partner Unitaid. The endTB partnership also is seeing strong results from an observational study, in addition to the clinical trial. The effort’s overarching goal is to find better, shorter regimens for hard-to-treat, multidrug-resistant TB (MDR-TB), using the first new TB medications in nearly 50 years—bedaquiline and delamanid.
A post-Soviet country of more than 18 million located in Central Asia, Kazakhstan is one of the world’s top five countries for both new and previously diagnosed cases of MDR-TB, according to the World Health Organization. It is also among the countries in the region hardest hit by COVID-19, with more than 110,000 confirmed cases and 1,300 deaths as of mid-August. Health officials fear that actual case and fatality numbers could be much higher than confirmed data.
“Given the situation, the Kazakhstan endTB team faced serious challenges to continue providing treatment to TB patients,” said Nataliya Morozova, program associate for PIH in Kazakhstan. “The team has urgently developed a set of measures to support patients in the settings of strict quarantine.”
A Bold Study
Standard, traditional tuberculosis treatments can last up to two years and include painful daily injections of drugs that can have multiple negative side effects, including temporary psychosis and hearing loss. The endTB trial tests five regimens and aims to show that bedaquiline and delamanid can offer patients a shorter course of treatment, with fewer side effects.
PIH and Kazakhstan’s National TB Program are collaborating to run the endTB trial with MDR-TB patients in the capital, Almaty. In Kazakhstan, TB patients normally are hospitalized for at least a few months at the beginning of care, with the goal of both containing the disease and properly administering treatment.
A total of 118 patients have participated in the trial in Kazakhstan, more than a fourth of the 463 patients in the endTB trial worldwide. Seventy of the Kazakhstan patients were continuing to receive treatment or follow-up as of mid-August. Some of the remaining 48 had already completed all procedures, while others had to withdraw from the study for various reasons.
COVID-19 Lockdown
From the beginning of the outbreak, Kazakh officials instituted severe measures to limit the spread of COVID-19. Since March 20, police set up roadblocks around Almaty. For more than two months the city was under lockdown, with many of its 2 million residents quarantined at home.
At the same time, a decision was made to empty TB wards and transform them into COVID-19 wards instead.

Raushanah Kuanysheva, a 23-year-old MDR-TB patient, was among those sent home. A self-employed marketing manager, she was diagnosed in January after suffering from severe pain in her upper back. An X-ray revealed an abnormality in her lungs. She was diagnosed with tuberculosis after a CT scan and sent to a hospital, where she was to undergo six months of treatment. However, Kuanysheva’s stay was cut short after just three months when the ward was transformed to care for coronavirus patients.
Initially, she received standard TB treatment. She said one of the drugs she was given was “really, really awful. It has negative effects on your mind.” At times, Kuanysheva said, she didn’t know who or where she was.
After two weeks, Dr. Amanjan Abubakirov, a TB specialist who works with PIH, offered her the opportunity to participate in the endTB clinical trial. She jumped at the chance, unafraid of the possible risks.
Her new regimen involves taking six medicines over nine months. She says none of them has caused serious side effects. When she was still at the hospital, specialists monitored her health, conducting weekly checks on her heart, vision, and hearing.
Video Treatment Support
The PIH team—including 10 trial coordinators and about 25 contracted hospital investigators, along with nurses and other support staff—used video treatment support (VTS) prior to the coronavirus pandemic. But now, it’s become an indispensable tool.
Kanat Khazhidinov, PIH research manager in Kazakhstan, said the team quickly switched all of the TB patients in the study from weekly hospital visits to receiving treatment via VTS.
The reasons were twofold: first, to minimize the risk of COVID-19 transmission between doctors and patients, and second, to accommodate patients who couldn’t leave their home or neighborhood due to the citywide lockdown. Virtual treatment has the added benefit for patients of avoiding stigma associated with a TB diagnosis.
“It was interesting that many patients didn’t want me or other physicians to visit them at home,” Abubakirov said. “Sometimes they are hesitant because their neighbors and relatives might spot the doctors.”
Still, Kuanysheva said maintaining her schedule of being constantly tested has been “really difficult, because of COVID.”
Every day, she receives a virtual visit from nurse Duysebayeva Nurgul, via WhatsApp. Over video, the nurse asks about her condition and watches as Kuanysheva takes all 12 of her pills, which can take some time as they are hard for her to swallow.
Kuanysheva also needs to have her sputum checked, so a nurse comes to her home monthly to retrieve a sample. She has her bloodwork done at a nearby lab.
Over time, her nurse and PIH team members have become trusted friends.
“I really appreciate them,” Kuanysheva said. “I’m really grateful for their support, not only for my TB situation.”
Checkpoint Medical Exams
While VTS covered a good portion of care, endTB trial patients still needed their medicines, and medical checks had to be performed to monitor possible side effects throughout the study.
Dr. Merey Otepbergenova, co-investigator of the endTB study in Kazakhstan, was one of several team members who traveled with her own vehicle, along with various examination tools and machines, to meet patients wherever possible.

In some cases, she made home visits, while other exams were performed at lockdown checkpoints. That meant an electrocardiogram and audiometry exam sometimes were conducted in the backseat of the doctor’s car, or a vision test was performed on the spot. When necessary, drugs were delivered directly to patients’ homes.
Due to his team’s determination, Khazhidinov said, “80 percent of all the activities within the endTB trial were accomplished during the lockdown.”
Abubakirov said he’s seen a big change in the effectiveness of care over his career as a TB doctor.
“In 2010, when I started, the situation was not favorable,” he said. “There were no effective TB drugs.”
New drugs started to arrive in 2016 and initially offered an effectiveness rate of about 40 percent.
Now, 75 percent of patients have favorable outcomes, Abubakirov said.
Dual Pandemics
The endTB trial is continuing, all while clinicians face the very real risk of contracting COVID-19. At the end of May, the Kazakhstan government loosened lockdown restrictions, only to see COVID-19 cases spike. New lockdowns followed.
Even that gap was perilous, however. In June, 11 of 15 core PIH staff members developed clinical symptoms of COVID-19. Abubakirov was among those who fell ill.
He was diagnosed with pneumonia, most probably due to COVID-19, although he was not tested. Twelve days later, he had recovered and was doing well. While some team members continued to work remotely, others took sick leave. After two weeks, no one from the team developed severe symptoms, and all have since recovered.
Abubakirov and his colleagues are just a few of the frontline, essential workers battling TB around the world. Now, in a cruel twist faced by health workers everywhere, they’re battling COVID-19, as well.
“The majority of these regimens were without an injectable, so people didn’t have to go to health facilities daily to get injected as part of their treatment,” Mitnick said. ”That certainly is helpful at a time when there is enormous pressure on health systems and TB services have been pretty much decimated by the COVID-19 outbreak.”
Article originally posted on pih.org
Learn more about the recent endTB observational study showing strong results for using new drugs and shorter treatment regimens to fight severe tuberculosis.



